AI Predictive Analytics: Optimizing Hospital Costs by 10% in 2026

The healthcare landscape in the United States is perpetually challenged by escalating costs, complex operational demands, and the imperative to deliver high-quality patient care. As we look towards 2026, the convergence of these challenges with rapid technological advancements positions Artificial Intelligence (AI) as a pivotal solution. Specifically, AI-driven predictive analytics is emerging as a game-changer, promising not just incremental improvements, but a significant 10% reduction in U.S. hospital costs through optimized resource allocation. This isn’t merely an optimistic projection; it’s a strategic imperative backed by tangible technological capabilities and a growing body of evidence demonstrating its profound financial impact.
The journey to achieving such ambitious cost savings is multifaceted, involving a deep dive into various operational domains within a hospital, from supply chain management and workforce scheduling to patient flow and equipment utilization. Each of these areas presents unique opportunities for optimization, and AI, with its capacity to process vast amounts of data and identify complex patterns, is uniquely positioned to unlock these efficiencies. This comprehensive exploration will delve into the mechanisms by which AI-driven predictive analytics can transform hospital operations, detailing the financial implications and outlining a roadmap for U.S. hospitals to embrace this technological revolution.
The Economic Imperative: Why U.S. Hospitals Need Cost Optimization
U.S. healthcare spending continues to outpace economic growth, creating a significant burden on individuals, businesses, and government budgets. Hospitals, as central pillars of the healthcare system, bear a substantial portion of these costs. Factors contributing to this include rising drug prices, increasing labor costs, administrative complexities, and the inherent inefficiencies within traditional operational models. The COVID-19 pandemic further exacerbated these pressures, highlighting vulnerabilities in supply chains, staffing models, and emergency preparedness.
In this challenging environment, every percentage point of cost reduction translates into substantial savings that can be reinvested into patient care, staff development, or infrastructure improvements. A 10% reduction, as targeted by AI-driven predictive analytics, represents billions of dollars annually across the U.S. hospital system. This isn’t about compromising care quality; it’s about eliminating waste, enhancing efficiency, and making smarter, data-driven decisions. The focus on hospital cost optimization AI is therefore not just about financial prudence, but about ensuring the long-term sustainability and accessibility of quality healthcare.
Understanding AI-Driven Predictive Analytics in Healthcare
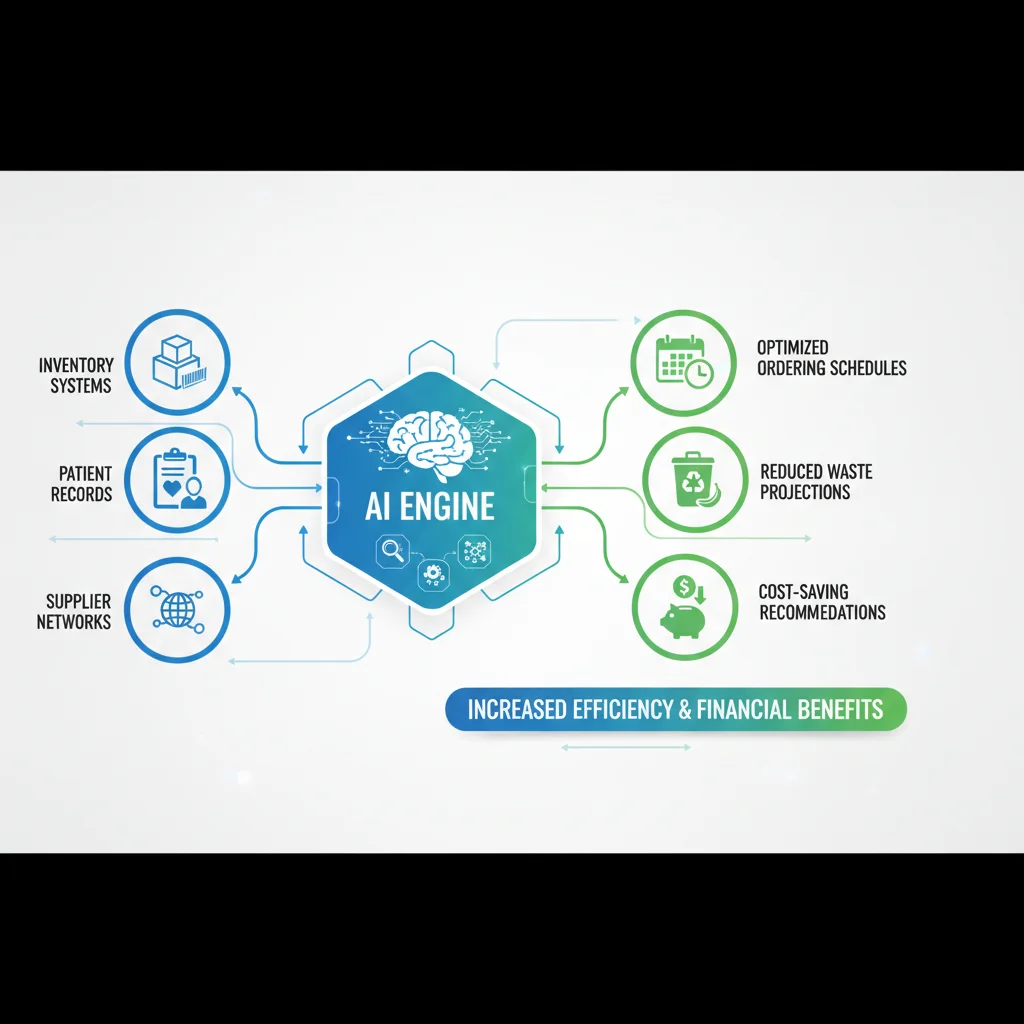
At its core, predictive analytics involves using historical data, statistical algorithms, and machine learning techniques to identify the likelihood of future outcomes. When applied to healthcare, this means anticipating patient needs, predicting equipment failures, forecasting resource demands, and optimizing operational workflows before issues arise. AI amplifies this capability by enabling the analysis of massive, diverse datasets – structured and unstructured – at speeds and scales beyond human capacity.
How AI Transforms Data into Actionable Insights:
- Data Aggregation and Integration: AI systems can ingest data from various hospital sources, including Electronic Health Records (EHRs), supply chain manifests, HR systems, billing records, and even external data like weather patterns or public health alerts.
- Pattern Recognition: Machine learning algorithms identify subtle patterns and correlations in this data that human analysts might miss, revealing underlying drivers of cost and inefficiency.
- Predictive Modeling: Based on identified patterns, AI builds models to forecast future events, such as patient admission rates, demand for specific medical supplies, or the likelihood of staff absenteeism.
- Prescriptive Recommendations: Beyond prediction, advanced AI can offer prescriptive advice – actionable steps hospitals can take to optimize outcomes, whether it’s adjusting staffing levels, reordering inventory, or rerouting patient flow.
The power of hospital cost optimization AI lies in its ability to move from reactive problem-solving to proactive prevention and optimization. This shift is fundamental to achieving the targeted 10% cost reduction by 2026.
Key Areas for AI-Driven Cost Reduction
To realize a 10% reduction in costs, AI-driven predictive analytics must be strategically deployed across several critical operational sectors within a hospital. Each area, while distinct, contributes to the overall financial health and operational efficiency.
1. Supply Chain Management and Inventory Optimization
Hospital supply chains are notoriously complex and often inefficient, leading to significant waste through overstocking, expired goods, or shortages that disrupt patient care. AI can revolutionize this by:
- Demand Forecasting: Predicting demand for specific medical devices, pharmaceuticals, and consumables based on historical usage, patient demographics, seasonal trends, and anticipated disease outbreaks.
- Inventory Management: Optimizing inventory levels in real-time, reducing carrying costs, minimizing waste from expired products, and ensuring critical supplies are always available.
- Vendor Management: Analyzing vendor performance, pricing trends, and contract compliance to identify cost-saving opportunities and negotiate better deals.
- Logistics Optimization: Streamlining ordering, delivery, and distribution processes within and between hospital facilities.
By preventing stockouts and overstocking, hospitals can significantly reduce expenditures related to emergency orders, storage, and waste. This is a prime example of where hospital cost optimization AI delivers immediate and measurable financial benefits.
2. Workforce Management and Staffing Optimization
Labor costs represent the largest expense for most hospitals. Understaffing can lead to burnout, decreased quality of care, and agency staff reliance (which is expensive), while overstaffing leads to unnecessary expenses. AI can optimize workforce management by:
- Patient Volume Prediction: Forecasting patient admissions, discharges, and specific care needs to accurately determine required staffing levels for different departments and shifts.
- Staff Scheduling: Creating optimized schedules that balance staff availability, skill sets, patient demand, and regulatory requirements, minimizing overtime and agency staff usage.
- Skill Gap Analysis: Identifying potential skill shortages or surpluses, allowing for proactive training or reallocation of resources.
- Predictive Maintenance for Staff Retention: Analyzing data to identify factors contributing to staff turnover, allowing hospitals to intervene and improve retention strategies.
The ability of AI to precisely match staffing to demand is crucial for both cost control and maintaining high standards of patient care. This direct impact on labor costs is a cornerstone of hospital cost optimization AI strategies.
3. Patient Flow and Throughput Optimization
Inefficient patient flow leads to longer wait times, increased length of stay, and reduced capacity, all of which have significant financial implications. AI can improve patient flow by:
- Admission and Discharge Prediction: Forecasting patient admissions and discharge times to optimize bed management and reduce bottlenecks.
- Operating Room (OR) Scheduling: Optimizing OR schedules to maximize utilization, minimize turnover times, and reduce idle periods.
- Emergency Department (ED) Throughput: Predicting ED patient volumes and acuity levels to allocate resources effectively, reducing wait times and improving patient experience.
- Resource Allocation: Dynamically allocating resources like diagnostic equipment, transport services, and clinical staff based on real-time patient needs and flow predictions.
By streamlining patient journeys, hospitals can increase capacity without expanding physical infrastructure, leading to significant cost savings and improved patient satisfaction.
4. Equipment Utilization and Maintenance
Medical equipment represents a substantial capital investment. Maximizing its utilization and ensuring its longevity through predictive maintenance can yield significant savings.
- Utilization Tracking: Monitoring real-time usage of expensive equipment to identify underutilized assets and optimize their deployment.
- Predictive Maintenance: Using sensor data and machine learning to predict when equipment is likely to fail, enabling proactive maintenance rather than costly emergency repairs or replacements.
- Capital Planning: Informing purchasing decisions for new equipment based on predicted future demand and existing asset performance.
This proactive approach minimizes downtime, extends asset life, and optimizes capital expenditure, directly contributing to hospital cost optimization AI goals.
Overcoming Implementation Challenges
While the benefits of AI-driven predictive analytics are clear, successful implementation requires addressing several key challenges:
- Data Quality and Integration: Hospitals often have siloed data systems with varying data quality. Integrating these diverse datasets into a unified, clean, and accessible format is a foundational step.
- Interoperability: Ensuring AI systems can seamlessly communicate with existing EHRs, supply chain software, and other hospital IT infrastructure is critical.
- Talent Gap: A shortage of data scientists, AI engineers, and clinical informaticists who can bridge the gap between technology and healthcare operations.
- Ethical Considerations and Bias: Ensuring AI algorithms are fair, transparent, and do not perpetuate or amplify existing biases in healthcare data.
- Change Management: Overcoming resistance to new technologies and processes among staff members. Effective training and communication are essential.
- Regulatory Compliance: Navigating complex healthcare regulations, including HIPAA, to ensure data privacy and security.
Hospitals must adopt a phased approach, starting with pilot projects in specific areas, demonstrating clear ROI, and then scaling successful initiatives across the organization. Strategic partnerships with AI solution providers can also help mitigate some of these challenges.
The Financial Impact: Quantifying the 10% Savings
Achieving a 10% reduction in hospital costs through hospital cost optimization AI by 2026 is an ambitious yet attainable goal. Let’s consider a hypothetical large U.S. hospital with an annual operating budget of $1 billion. A 10% reduction would translate to $100 million in annual savings. These savings can be broken down across the previously discussed areas:
- Supply Chain (Estimated 2-3% of total budget): A 10-15% efficiency gain in supply chain could yield $2-4.5 million in savings.
- Labor Costs (Estimated 50-60% of total budget): Even a modest 2-3% improvement in labor efficiency through optimized staffing could save $10-18 million.
- Patient Flow/Throughput (Indirect costs, but significant): Reducing length of stay, improving OR utilization, and decreasing ED wait times can free up capacity, allowing for more patients to be treated without additional infrastructure, potentially leading to increased revenue or avoiding capital expenditures. This could indirectly save tens of millions.
- Equipment Management (Capital expenditure and maintenance): Predictive maintenance and optimized utilization can lead to significant savings on repairs, replacements, and extended asset life.
- Reduced Administrative Overhead: AI can automate many administrative tasks, reducing the need for manual processing and improving accuracy in areas like billing and coding.
These figures are illustrative but highlight the immense potential. The cumulative effect of numerous small to medium optimizations across various departments, driven by AI’s holistic view of hospital operations, is what will ultimately lead to the 10% target. The return on investment (ROI) for AI implementation can be rapid, often within 12-24 months, making it a compelling financial proposition.

The Future of Healthcare: Beyond Cost Savings
While the focus here is on cost optimization, it’s crucial to recognize that the benefits of AI-driven predictive analytics extend far beyond financial savings. Improved resource allocation directly translates to:
- Enhanced Patient Outcomes: Better staffing, timely access to equipment, and efficient patient flow contribute to higher quality care, reduced medical errors, and improved patient safety.
- Improved Staff Satisfaction: Optimized schedules, reduced burnout, and better resource availability can lead to a more satisfied and engaged workforce.
- Increased Capacity and Accessibility: More efficient operations mean hospitals can serve more patients without necessarily expanding physical infrastructure, improving access to care in communities.
- Data-Driven Decision Making: Leaders gain unprecedented insights into their operations, enabling more strategic planning and adaptive management.
The synergy between financial health and clinical excellence is profound. Hospitals that embrace hospital cost optimization AI today will be better positioned to navigate the complexities of tomorrow’s healthcare environment, offering superior care while maintaining financial stability.
Case Studies and Early Successes
While a universal 10% cost reduction by 2026 is an aggregate goal, individual hospitals and health systems are already reporting significant successes with AI-driven predictive analytics:
- University of Pittsburgh Medical Center (UPMC): UPMC has leveraged AI to optimize bed assignments, reducing patient wait times and improving throughput, leading to more efficient resource utilization.
- Mayo Clinic: Mayo Clinic has explored AI for predictive analytics in various areas, including forecasting patient no-shows and optimizing appointment scheduling, which directly impacts revenue and resource allocation.
- Cedars-Sinai Medical Center: This institution has implemented AI to predict patient deterioration, allowing for early intervention and potentially reducing costly critical care admissions. While not directly cost-saving in the same way as supply chain, preventing adverse events has significant financial and clinical benefits.
- Kaiser Permanente: Kaiser has used predictive models to identify patients at high risk of readmission, enabling targeted interventions that improve patient outcomes and reduce the financial burden of readmissions.
These examples illustrate that the technology is mature enough to deliver tangible results. The challenge now is to scale these individual successes into a systemic transformation across the U.S. hospital landscape.
The Roadmap to 2026: A Strategic Approach
For U.S. hospitals aiming to achieve the 10% cost reduction target by 2026, a clear strategic roadmap is essential:
- Assess Current State: Conduct a thorough audit of existing operational inefficiencies, data infrastructure, and technological readiness. Identify high-impact areas for initial AI deployment.
- Develop a Data Strategy: Prioritize data governance, quality improvement, and integration efforts. Establish a robust data architecture that can support AI initiatives.
- Invest in Talent and Training: Recruit or train staff with expertise in data science, AI, and clinical informatics. Foster a culture of data literacy and continuous learning.
- Start Small, Scale Smart: Begin with pilot projects in well-defined areas (e.g., specific department’s supply chain or ED throughput) to demonstrate ROI and build internal champions.
- Choose the Right Partners: Collaborate with experienced AI vendors who understand the nuances of healthcare and can provide scalable, secure, and compliant solutions.
- Monitor and Iterate: Continuously track the performance of AI models, gather feedback, and iterate on solutions to ensure ongoing optimization and adaptation to changing conditions.
- Foster a Culture of Innovation: Encourage experimentation and a willingness to embrace new technologies. Leadership buy-in is paramount for successful transformation.
By following this roadmap, hospitals can systematically integrate hospital cost optimization AI into their core operations, paving the way for significant financial improvements and a more resilient, patient-centric healthcare system.
Conclusion
The aspiration of cutting U.S. hospital costs by 10% through AI-driven predictive analytics by 2026 is not a distant dream but a tangible goal within reach. The technology is here, the economic imperative is undeniable, and early successes demonstrate its transformative power. By strategically deploying AI across supply chain, workforce management, patient flow, and equipment utilization, hospitals can unlock unprecedented efficiencies, reduce waste, and reallocate resources where they are most needed – at the patient’s bedside.
This shift towards intelligent, data-driven healthcare operations is not just about financial savings; it’s about building a more sustainable, resilient, and higher-quality healthcare system for all. The hospitals that embrace this technological evolution now will be the leaders of tomorrow, setting new benchmarks for efficiency, innovation, and patient care. The future of healthcare is intelligent, and AI-driven predictive analytics is the key to unlocking its full potential.





